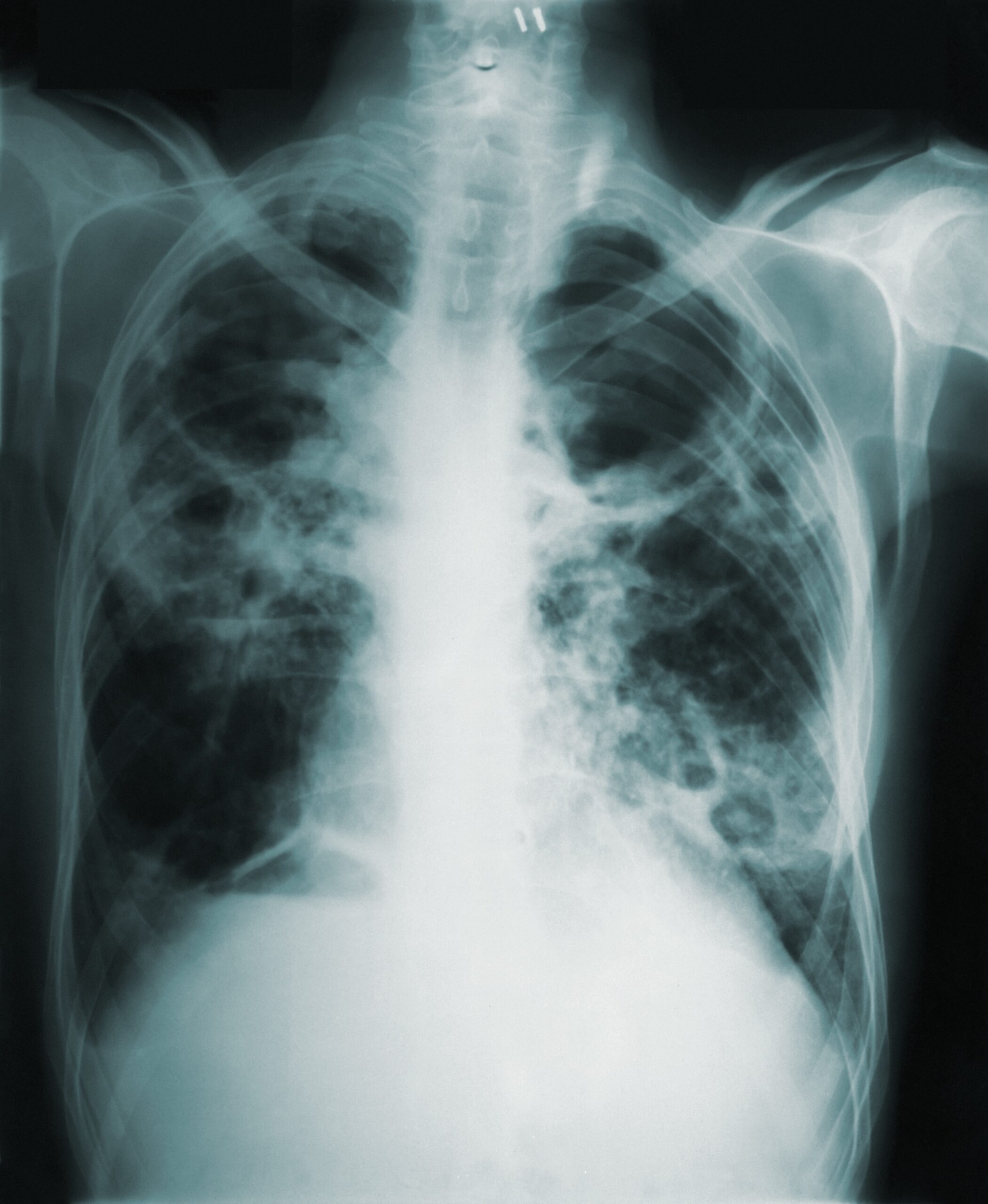
On the 24th of March 1882, 141 years ago to the day, Dr Robert Koch announced his discovery of Mycobacterium tuberculosis, the bacterium that causes tuberculosis (TB). Just over 60 years later, the first TB treatment was developed, and a course now costs less than 10 USD. Despite this, TB remains responsible for more deaths worldwide than any other single-agent infectious disease, killing 1.6 million people every year – more than homicide, conflict, malaria, typhoid and cholera combined.1–7
Over the last 100 years, high-income countries have witnessed drastic reductions in TB incidence thanks to improved living standards, established healthcare infrastructures and successful Bacillus Calmette–Guérin (BCG) vaccine programme implementation. On the flip side, low- and middle-income (LMICs) countries are continuing to struggle to make similar progress. Statistics show that TB is a disease of the disadvantaged, and although a degree of progress has been made in reducing TB incidence in LMICs, today, being World Tuberculosis Day, we should collectively acknowledge the significant action that must be taken if we are to achieve the World Health Organization’s ambitious target of eradicating TB by 2030.
Improving detection and increasing diagnosis
A primary focus of any disease eradication strategy must be to identify all existing cases. Between a quarter and a third of the world’s population is estimated to be infected with TB; however, around 4.1 million estimated new TB cases were not reported in 2020.1,8
Such disparity can be attributed to various healthcare barriers, including a lack of TB diagnostic laboratories in rural health facilities, an absence of a standard referral system to municipal hospitals for further assessment, substandard training and suboptimal standard operating procedure (SOP) design and implementation, as well as a fear of infection that is intensified by hindered access to personal protective equipment (PPE). By providing LMICs’ sub-municipalities with at least one diagnostic facility each, and ensuring staff are offered both sufficient training and appropriate PPE, many of the barriers to early diagnosis can be overcome and necessary treatment can be distributed accordingly, helping us move one step closer to the WHO’s 2030 goal.
Giving precedence to paediatric cases
Children and adolescents make up a significant proportion of undiagnosed TB cases, and this is particularly concerning given that they have a significantly increased risk of disease progression following infection, as well as a 66% higher mortality rate compared to TB-infected adults.1,9 This subset of patients also typically demonstrate poor compliance with TB therapy and tend to congregate in group settings, which can accelerate disease transmission.
The problem is further exacerbated through the various challenges associated with paediatric and adolescent TB diagnosis, including children’s inability to produce sputum for the purpose of testing and a high patient-to-healthcare worker ratio that puts a strain on scarce resources.1 Furthermore, in a survey conducted in 2015, the lack of appropriate child-friendly drug formulations was named by country representatives as the most common challenge, and the difficult diagnosis of pediatric and adolescent TB was cited by 10 out of 35 surveyed LMIC countries.10
In December 2015, WHO and the Global Alliance for TB Drug Development collaborated to launch child-friendly fixed-dose combinations for the treatment of drug-susceptible TB in children weighing <25 kg, which has resulted in considerable progress in treatment availability within Europe.10 If the same strategy were to be applied to LMICs outside of Europe, and pediatric diagnosis were prioritized through various interventions, such as directing BCG vaccinations to children (especially in high-risk groups) and mobile health screening in rural areas, those most vulnerable could be protected from disease progression and transmission rates slowed.
Prioritizing prevention
Interventions that aim to increase preventive treatment uptake are likely to have a greater impact on TB control and elimination than those focussing on improving completion of treatment by patients. Latent TB infection (LTBI), which typically occurs during the time following infection but prior to the onset of symptomatic disease, presents a perfect window of opportunity for disease prevention. Although highly effective, preventive therapy has previously been limited to high income countries; however, over recent years, access has been extended globally.
That being said, implementation of preventive therapy remains sluggish, especially in young children, with just 23% of eligible children under 5 receiving TB preventive care.1 The same issues associated with pediatric TB treatment translate into preventive care. Additionally, LTBI is diagnosed by the tuberculin skin test or interferon-gamma release assay, both of which can be challenging to use.11
In order to overcome such obstacles, high-risk populations, such as those living with HIV or those living with an individual with confirmed TB, must receive timely screening for TB, a strategy for implementation of BCG vaccination of children must be put in place, and healthcare workers in LMICs must be provided with appropriate training and PPE. Additionally, providing cash to LMICs can facilitate the purchasing of necessary testing equipment and ensure access to adequate treatment.
World Tuberculosis Day offers us an ideal opportunity to raise awareness of the devastating effects of the disease while also recognizing the various barriers that are preventing the realization of the WHO’s 2030 eradication goal. By improving detection and diagnosis, prioritizing pediatric cases, especially those with LTBI, and taking steps to improve preventive measures within LMICs, countless lives could be saved, which is why this month, we have decided to donate to the Stop TB Partnership, an organisation dedicated to making TB diagnosis and treatment available for all, regardless of socioeconomic status.
- Szkwarko D, et al. R I Med. 2019;102(7):47–50.
- Our World in Data. Homicides. Available at: https://ourworldindata.org/homicides. Accessed March 2023.
- Fact Sheets: Malaria. Available at: https://www.who.int/news-room/fact-sheets/detail/malaria. Accessed March 2023.
- Our World in Data. Total conflict-related civilian deaths, World, 2015 to 2021. Available at: https://ourworldindata.org/grapher/total-conflict-related-civilian-deaths?country=~OWID_WRL. Accessed March 2023.
- Typhoid. Available at: https://www.who.int/health-topics/typhoid#tab=tab_1. Accessed March 2023.
- Cholera worldwide. Available at: https://www.ecdc.europa.eu/en/all-topics-z/cholera/surveillance-and-disease-data/cholera-monthly. Accessed March 2023.
- Fact sheets: Tuberculosis. Available at: https://www.who.int/news-room/fact-sheets/detail/tuberculosis. Accessed March 2023.
- Asemahagn MA. Infect Drug Resist. 2022;15:1947–1956.
- Lönnroth K et al. Eur Respir J. 2015;45:928–952.
- Gröschel MI, et al. Eur Respir J. 2019;28:180106.
- Harries AD, et al. F1000Res. 2018;7:F1000 Faculty Rev-1011.